Gateshead © Am Ang Zhang 2017
Kirsty was a beautiful six-month-old baby girl in whom fate had installed a lethal self-destruct mechanism, a miserable detail that seemed destined to end her life before her first birthday. ALCAPA is an abbreviation for Anomalous Left Coronary Artery from the Pulmonary Artery, an isolated and exceptionally rare congenital anomaly in the overall complexity of human anatomy.
Simply put, it's bad wiring. Both coronary arteries should rise out of the aorta and supply the heart muscle with well-oxygenated blood under high pressure. They should never be attached to the pulmonary artery, as this has both low pressure and poor oxygen content. Early survival with ALCAPA therefore depends on the development of new "collateral" blood vessels between the normal right coronary artery and the misplaced left coronary artery. But these eventually are insufficient to sustain blood flow to the main pumping chamber.
Muscle cells deprived of oxygen die and are replaced by scar tissue, leaving baby to suffer what are in effect repeated, painful heart attacks. Scar tissue stretches, causing the left ventricle to dilate, then the heart progressively fails and the lungs become congested with blood, leading to breathlessness and exhaustion. Even during feeding.
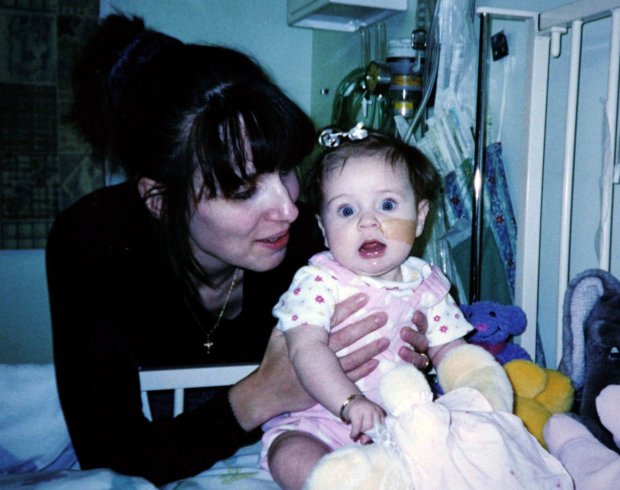
Kirsty Collier with her mum Becky before her operation. After having a third of her heart removed in pioneering surgery Kirsty astounded medical experts by making a ''miracle'' recovery. SWNS.com
But because ALCAPA is exceedingly rare, the diagnosis is seldom made until the infant is terminally ill. Fortunately, her parents were intelligent, had recognised that there was a serious problem and were persistent in finding help for her.
Kirsty's story was particularly harrowing. Her mother Becky already had a three-year-old son and was an experienced and responsible mum. All antenatal checks and ultra-sound scans had appeared normal. Kirsty was born on August 21, 1998, by elective Caesarean section with a spinal anaesthetic and at first everything seemed normal. But not for long.
In the womb, the pressures and oxygen content of the aorta and pulmonary artery are the same, so Kirsty's tiny heart was safe. After birth, the circulations to the body and newly expanded lungs separate, and both pressure and oxygen content in the pulmonary artery fall. So, in cases of ALCAPA, both blood flow and oxygen content in that critically important left coronary artery fall precipitously, too.
Kirsty was grunting even during the first attempt to breastfeed in the hospital, and Becky noticed beads of sweat trickling from the bridge of her baby's nose. The effort of feeding repeatedly made her fractious and distressed.
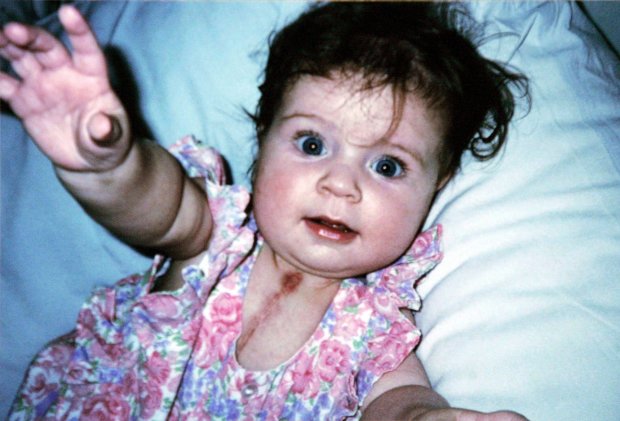
Kirsty Collier two months after her operation in February 1999. Kirsty had a third of her heart removed when she was just 4 months old. SWNS.com
This was distinctly different from how her son had been, so Becky asked for a paediatrician to review Kirsty. She was told that there was absolutely nothing to worry about but the truth was that no one had bothered to find out what was wrong.At this stage, Becky had little choice but to take her irritable but precious little bundle home.
Within weeks Becky was certain that something was seriously amiss, because during every feed there was sweating and vomiting. Kirsty struggled for breath, clenched her little fists and screamed until she was puce in the face. Together they made many visits to the GP, sometimes as many as three times a week, but they always received the same non-committal reassurance – tense, unpleasant encounters, as Becky was deemed neurotic and unable to cope.
Despite Kirsty's rapid breathing she had no temperature. Chest infections were ruled out, and her belly was soft, with no signs of stomach or intestinal blockage. All of the common paediatric problems were excluded. Becky became more and more anxious. Kirsty wasn't gaining weight. She had a pasty, washed-out look and a cough like a dog's bark.
In reality this baby was suffering repeated small heart attacks with excruciating chest pain that she could neither communicate nor understand. The human body can be outlandishly cruel.
Kirsty as a 10-year-old with her mother Becky Collier. SWNS.com
Eventually, after a meltdown in the GP's surgery, Becky insisted that Kirsty should be referred to the local hospital. Twice she had chest X-rays, only to be diagnosed with bronchiolitis – inflamed breathing tubes – on both occasions. Then one day during her afternoon nap Kirsty turned a terrible slate-grey colour. She was barely rousable and limp. Becky snatched her up and rushed to the surgery. But by the time they presented themselves at the receptionist the baby was awake and pink again.
Becky was told to stop fussing and that there were children to be seen who were actually sick. On this occasion mother and child were acrimoniously dispatched, once more with a prescription for antibiotics. Kirsty's enormous heart remained undetected.
This time, Becky drove directly to the accident and emergency department of her small local hospital. They were seen by a sympathetic female doctor who had children of her own. Recognising that a mother's instinct was usually correct, she referred them on to a larger city hospital for review by the on-call paediatrician.
It was a bitterly cold, frosty night and they were left sitting in an unheated hospital corridor for several hours. Becky frantically struggled to keep Kirsty warm but she became progressively more limp and grey. Eventually, late into the night, they were seen. The first junior doctor suggested bronchiolitis and intended to dismiss them without investigation.
Beckyrefused to leave without a chest X-ray. She was told off for her unreasonable attitude – how thoughtless to inconvenience the hard-pressed duty radiographer at that time of night. So the sad pair were dispatched unescorted down poorly lit corridors and icy outside walkways to find their own way to the X-ray department. It was well past midnight when they returned, clutching the tell-tale picture, which Becky presented to a nurse. They were parked once more.
Another thirty minutes passed, then a dramatic shift in attitude from the hospital staff. Now there were hushed voices, grave expressions, and nurses bringing drips and drugs. The previously mean, now embarrassed nurse took Becky aside to explain that Kirsty was being transferred to the specialist children's heart unit in Oxford. By ambulance this time.
So what did the X-ray show to trigger this frenzy of activity? Kirsty had a massive heart. Her problem was immediately obvious on the X-ray film. When the staff were pressed about her previous X-rays at the same hospital, Becky was told that the heart shadow had been misinterpreted as fluid. Some mistake!
In Oxford, the paediatric cardiology registrar met the ambulance and took them directly to a ward packed with children with serious heart problems and beeping monitors – a hive of activity in the depths of night.
Kirsty with her parents before her school prom. Kirsty made a full recovery and aside from a feint scar on her chest has little to show for the surgery. Supplied
Nick Archer arrived at 3am. An ECG and blood tests were done quickly, then the echo machine was brought in to image Kirsty's heart chambers. First it seemed like good news. All four chambers were there, with no holes between them. But worryingly the left atrium and ventricle were both enlarged, the ventricle dramatically so. This explained the heart failure and accounted for the striking chest X-ray.
In little more than an hour, the cardiology team established that Kirsty had severe heart failure from multiple heart attacks. Parts of the left ventricular wall now consisted of thin scar tissue interspersed with poorly contracting muscle, a rare condition in an infant but one that provided the likely diagnosis. One further test was needed. A cardiac catheter would confirm the diagnosis but would require a general anaesthetic, so she'd have to be in much better condition before proceeding.
It was a full five weeks before Becky's baby was considered fit enough for the cardiac catheter. The evening before the operation, the anaesthetist came round to talk. Normally a jolly and optimistic character, on this occasion he didn't have much to smile about. That night, Kirsty was christened in her cot by the hospital chaplain, the doctors, nurses and other families gathering around the bed to support them.
That morning, Becky dressed her baby in her best pyjamas and tied a bow in her hair for her trip to the catheterisation laboratory. Ironically it was Valentine's Day. As Becky put it to me later, "A girl has to look her best, even when she's poorly.":
Once I was on the plane home I started to sketch the anatomy of Kirsty's aorta, pulmonary artery and abnormal left coronary artery. I knew that the current techniques in operations for ALCAPA had limitations and a substantial failure rate, so I used my time during the flight to work out an alternative. By the time we were cruising high above Java, I'd designed my new operation.
I called my colleague Takahiro Katsumata when I got back to Oxford and asked him to bring Kirsty's parents to my office with a consent form. The cardiac catheter had shown precisely what Archer had suspected. Kirsty needed surgery as soon as possible.
Becky looked tired and drawn when I saw her.
I don't do transmitted anxiety if I can help it. But it's much more difficult for my anaesthetist colleagues who have to deal with the agonising separation when the patient is given over to them.
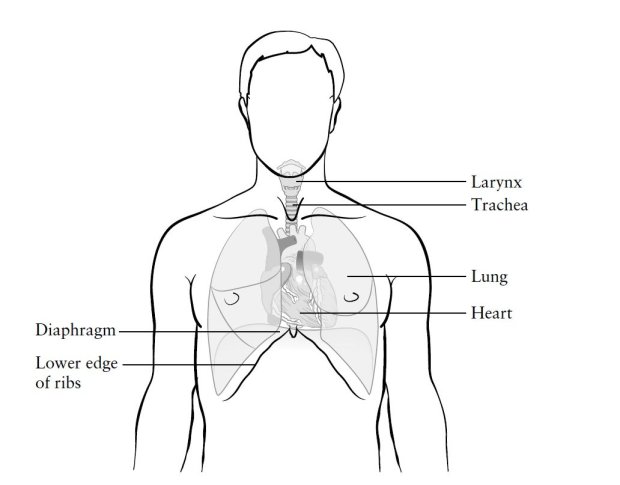
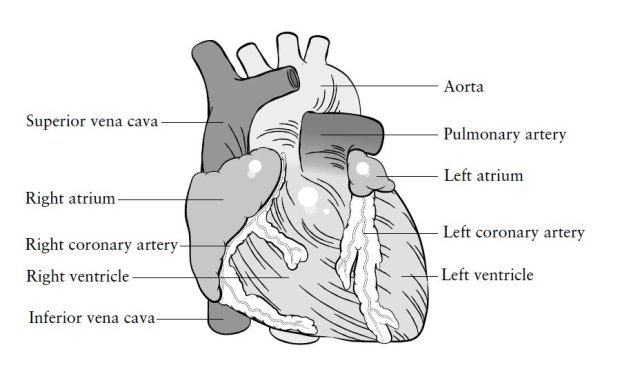
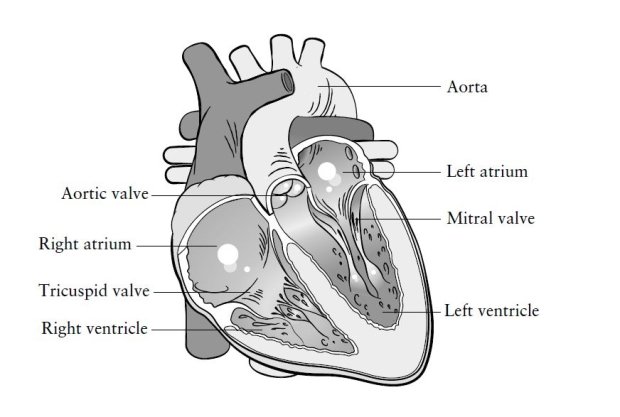
FRAGILE LIVES Illustrations labeling and depicting elements of the heart and cardiovascular systems. Heart Surgery Prodger, Isabel
I described my planned operation to the team and explained why I felt it would be an improvement on existing techniques. The new left coronary artery would be constructed with a flap of aortic wall that would sit below a corresponding pulmonary flap to make a tube, the latter containing the misplaced origin of the left coronary artery at its apex. The product would be a new coronary artery delivering high-pressure, well-oxygenated blood directly from the aorta, where it should have come from in the first place. Blood fully saturated with oxygen would then supply the failing heart muscle and prevent further heart attacks. Katsumata was intrigued and excited by my proposed approach, so much so that he rushed off to call the hospital's film crew.
The risks of the operation were substantial. Becky's shaky hand signed the consent form and I walked back with them to the children's ward. When we reached the cot, Kirsty's heart failure was worse than I imagined. She was emaciated, her heaving ribs and rapid breathing a consequence of her congested lungs, and her abdomen swollen with fluid. Without immediate surgery she'd be dead within days. Although a voice in my head screamed, "Oh shit," my mouth correctly said, "I'll go to theatre now."
The anaesthetist knew the score, having already anaesthetised Kirsty for the cardiac catheterisation, and some of the monitoring lines were still in place.
"Do you really think you can get this baby through?" was his opening line.
I didn't reply, bidding a cheery "Good morning" to the nurses and perfusion team in the operating theatre, then went straight to the coffee room. I wanted to avoid seeing Becky leave her baby with strangers, always an excruciating event.
When I returned, Kirsty was already on the operating table, covered in green drapes held in place with an adherent plastic drape. All that was visible were her bony little chest and swollen abdomen. Heart surgery needs to be an impersonal, technical exercise.
I joined Katsumata and my six-foot, six-inch Australian colleague Matthew at the scrub sink. While we scrubbed in silence, the film camera was carefully positioned next to the operating lights. There was a palpable buzz of excitement. We were about to do something novel, esoteric and risky.
There was no bleeding as I drew the scalpel blade along the skin over Kirsty's breast bone. In shock, her skin capillaries had shut down to divert blood to vital organs. Next, the electrocauter cut through the thin layer of fat onto the bone, producing its characteristic buzzing noise accompanied by a whiff of burning as the current cauterised the oozing blood vessels, although this time there were few of these. Then the electric saw cut through the length of her sternum, exposing bright red bone marrow.
FRAGILE LIVES Illustrations labeling and depicting elements of the heart and cardiovascular systems. Heart Surgery Prodger, Isabel
We used a small metal retractor to crank open her tiny chest, bending and stretching the joints between the ribs and the spinal column. In babies, the fleshy thymus gland lies between the sternum and the fibrous sac around the heart, but by now it had done its work producing antibodies for the foetus so we removed it.
The electrocauter continued its messy but vital work, cutting through the fibrous pericardial sac to expose the heart, straw-coloured fluid pouring out and being drawn away by the sucker. Meanwhile the other members of the team worked on silently. The anaesthetist gave heparin to stop Kirsty's blood from clotting in the heart–lung machine, the perfusion team set up the complex array of tubing, pumps and oxygenating equipment to keep Kirsty's body alive when her heart was stopped, and the scrub nurse concentrated on having the correct surgical instruments ready to slap into my palm. I rarely had to ask for anything.
As we pulled up the edges of the pericardial membrane to display the heart, Katsumata – in a moment of wry Japanese humour in times of stress – involuntarily uttered what now had become our surgical catchphrase, "Oh shit, don't mention the war." Back from his first cigarette, the anaesthetist popped his head over the drapes in response to Katsumata's comment. Others could see it all on the video screen.
What should have been a walnut-sized heart was revealed to be the size of a lemon. The enlarged right coronary artery was obvious, its many inflated branches crossing over towards the left ventricle. While the right side of the heart pumped vigorously against raised pressure in the lungs, the left ventricle was hugely dilated and barely moved.
Batches of newly necrotic muscle merged with areas of white, fibrous scar tissue, the result of the many small, painful heart attacks endured by Kirsty during her first six months of life. But Kirsty had survived to this point and it was our job to keep it that way.
Having exposed this heart I began to question the wisdom of attempting such a complex operation having come straight from a day-long flight.
But urgent heart transplants were virtually impossible in babies; this replumbing of her heart's blood supply was her only chance of life.
Tiny pipes were inserted to connect her to the heart–lung machine, and I then gave the signal to continue. The perfusion technician turned on the roller pump and Kirsty's heart gradually emptied. At this point, technology had taken over, diverting blood away from her lungs and into the synthetic oxygenator.
FRAGILE LIVES Illustrations labeling and depicting elements of the heart and cardiovascular systems. Heart Surgery Prodger, Isabel
With her empty heart still beating I cut through the pulmonary artery above the origin of the anomalous coronary, which sat there like the pearl in an oyster. Now we had to connect it without tension to the high-pressure aorta that lay an inch away. The conventional method was simply to trying to stretch and re-implant the origin of the vessel into the side of the aorta. But this could result in thrombosis and blockage, so I pressed on with my new technique.
This delicate exercise could only be achieved by clamping the aorta and temporarily stopping all blood flow to the heart. We'd protect the muscle by infusing cardioplegia fluid directly into both coronary arteries, flushing all the blood out and collapsing the ventricle like a punctured football. This induced state of inactivity, common in heart surgery, is reversed simply by removing the clamp on the aorta, which allows blood from the heart–lung machine to flow back into the coronary arteries.
For the reconstruction of this tiny vessel, the stitching had to be precise, accurate and watertight. The procedure went well. Just thirty minutes after the heart was stopped, the conjoined flaps restored Kirsty's coronary artery anatomy to what it should have been.
As the clamp was removed, bright red oxygenated blood – rather than de-oxygenated blue blood – flooded the left ventricular muscle. Her heart changed from a pale pink colour to deep purple, then became almost black in parts. Before re-constructing the pulmonary artery we checked that there was no bleeding from the lines of stitching behind it. Soon the electro-cardiogram showed uncoordinated electrical activity, and the heart stiffened with renewed muscle tone.
Unusually for a child, her reperfused heart kept writhing and squirming in ventricular fibrillation. We used an electric shock directly through the muscle to restore normal rhythm. Ten volts – zap! The heart defibrillated and stopped wriggling. It was now motionless but we expected a normal rhythm to resume at any moment.
But it didn't. The purple ball fibrillated and squirmed again, and the anaesthetist's head popped over the drapes to request the obvious – "Shock it again!" We did and the same thing happened. It wasn't coming back.
This was serious electrical instability caused by the scar tissue, so we gave the appropriate drugs to stabilise the muscle cell membranes.
"Let's give it more reperfusion time," I told the anaesthetist.
"OK, I'll go out for a fag then," he said.
Twenty minutes later we tried again. Twenty volts – zap! This time her whole little body levitated from the operating table and her heart defibrillated. Although it slowly began to beat, it was barely more than a flicker. Ominous, but we had drugs in reserve to make it pump harder.
I asked the anaesthetist to start an adrenaline infusion and told the perfusionist to cut back on pump flow to leave some blood in the heart. This was operating theatre protocol, and it's just like the military. You make a request to a medical colleague but give orders to the technical staff. If you start giving orders to an anaesthetist they'll tell you to piss off, and will go off and do something different.
My gaze remained fixed on Kirsty's pathetic little heart. The new coronary artery was fine – there was no kink in the tube and no bleeding. For the first time, the left ventricle was receiving well-oxygenated blood at the same pressure as the rest of the body. But her heart still looked like an overripe plum and was barely beating at all. What I was thinking was we're stuffed, this heart's had it; great operation – dead baby.
Of course, I didn't let the others know my thoughts but I was starting to fade. I suggested that the cameraman should stop filming for a while because nothing was going to change and asked Katsumata to come to my side of the operating table while I took a break.
I removed my gown and gloves, and went to make a call in the anaesthetic room. Mike followed.
"Can you repair it?" he asked me.
"Don't think so."
"I'll get Archer to warn the parents, then."
I slumped on a stool and picked up the phone. One of the lovely nurses put a coffee and doughnut in front of me.
In five minutes, Archer was down from his outpatient clinic at the theatre door. He didn't need to ask.
My bladder was full and I wandered off to the loo. When I got back, my brain had regained control without that distraction and I now really needed to focus. What, if anything, could I do to make things better? I was running out of ideas.
The left ventricle was scarred, dilated and now globular – not the normal elliptical shape. This distortion had pulled open the mitral valve and prevented it from closing. As the left ventricle tried to pump blood around the body as much as half of it flowed backwards to the lungs. Heart function is always temporarily worsened during surgery, but in Kirsty's case it seemed terminal. I'd hoped that resting the heart on the bypass machine would help it to recover. It hadn't.
I went back to the operating theatre, scrubbed up again and switched with Katsumata. He said nothing, but looked crestfallen – a clear message. I asked the anaesthetist to start ventilating the lungs and told the perfusionist to prepare to slowly ease off the machine. At this point, Kirsty's heart needed to take over and support the circulation, otherwise she'd die on the operating table. We all stared at the traces on the screen, hoping to see her blood pressure rise. It briefly reached half normal, but then fell away rapidly as the pump was switched off.
"Shall we go back on?" asked Katsumata.
Watching the left ventricle flicker on the echo, the perfusionist questioned whether it was worth it.
I wasn't yet ready to call it. Failure would mean death for the little girl and a life of torment for the parents.
"Let's go back on, give it another half hour."
This in itself was problematic, as a long bypass time always lessened the chance of recovery.
Kirsty's parents were waiting in the children's ward – Archer had gone to warn them. When we called him back, Becky insisted on coming to the doors of the operating theatre complex with him. Should I tell her that the heart was too badly damaged, that the diagnosis should have been made months ago and that Kirsty had been let down by an overburdened system?
On the very rare occasions that a child died on the operating table I always talked to the parents myself. It was something I dreaded, the very worst part of my job.
The entrance to the theatre complex opened automatically onto the hospital corridor. I was immediately confronted by eyes full of grief and desperation. I remember Becky saying, "Please save my little girl." I was pole-axed. I turned back to the sombre theatre, put on a new mask and scrubbed up again.
The anaesthetist had finished yet another cigarette, and said, "Things are no better. Can we turn the pump off?"
"No, I'm going to try one more thing. Turn the lungs off. Run the camera again."
This was my last-gasp attempt. It was something that could only be justified by invoking the laws of physics and had never been done before in a child. The tension on the wall of Kirsty's scarred left ventricle was elevated because of the size of the cavity. From a recent conference, I knew that a Brazilian surgeon had made a series of failing adult hearts smaller when a tropical infection, Chagas disease, had weakened the muscle. The operation had been attempted for other types of heart failure patients in North America but was quickly discredited and abandoned. In my view, this bold approach was Kirsty's last hope.
I was not going to risk stopping the heart again, so I took a glistening new scalpel and cut the beating left ventricle wide open from apex to base, just like unzipping a sleeping bag. I began in an area of scar, carefully avoiding the muscles that support the mitral valve, and the filleted heart immediately fibrillated in response to cutting. This was fine because there was no risk of it pumping air.
Frankly, I was stunned by the unexpected appearance of the inner lining of the heart. It was covered in thick, white scar tissue. To reduce the diameter of the ventricle I cut away the scar tissue on either side of the incision until I reached bleeding muscle and then removed one third of the circumference of the chamber.
In an attempt to stop the mitral valve from leaking I sewed the central point of its two leaflets together, turning it from an oval to a double orifice structure resembling a pair of spectacles. Then I simply sewed the muscle edges together with a double row of stitches to close the heart. In the end, this much smaller heart looked like a quivering black banana. Not for a moment did I think it would ever start again – and nor did my colleagues. Most of them thought I was crazy.
Word of the bizarre operation in Theatre 5 soon spread. The curious gathered to watch and the camera kept on filming. We had to ensure that all air was removed from the heart, otherwise it could be ejected into the blood vessels of the brain and cause a stroke. After that, all that remained was to defibrillate and try to restore normal heart rhythm.
"We're done," I announced. "Try 20 volts."
Zap! The heart stopped quivering, and for what seemed like an age there was no spontaneous electrical activity. I poked the muscle with forceps and it contracted in response. This time there was a flicker on the blood pressure trace. Miraculously, the black banana had ejected blood into the aorta.
The anaesthetist looked again at the echo. "It certainly looks different. Shall we try using the pacemaker?"
I was already sewing the fine pacing wires into place. We arbitrarily set the pacing box rate at 100 beats per minute and switched it on. I told the perfusionist to cut back on the pump flow rate and leave blood in the heart to see if it would eject consistently. It did. What's more, the echo showed that the mitral valve no longer leaked. At this point I felt that we were in with a chance. Life really does depend upon physics and geometry.
It was now after midday. Kirsty had been on the bypass machine for more than three hours and we needed to get her off it. As if timed to perfection, her own heart rhythm suddenly broke through the pacing. Coordinated natural heart rhythm is much more efficient than electrical pacing, providing much better blood flow and pressure.
It was like switching on a light in the operating theatre. Gloom changed to elation, adrenaline kicked in and my fatigue suddenly lifted. We gave Kirsty an infusion of adrenaline to help her heart take over from the bypass machine. Finally I gave the instruction to"'come off slowly". We still expected her blood pressure to fade, yet the curiously reconfigured little heart kept on pumping.
I remained silent, but I looked over my mask at Katsumata. He knew that I'd had enough by now. "Let me finish," he said.
I took a last, disbelieving glance at the little black banana pumping away, then turned to the echo screen, where the incomprehensible flashes of white, blue and yellow were also reassuring, like a blazing fire. We could see blood streaming through the new left coronary and a double jet entering the left ventricle through the mitral valve – a curiously reconfigured baby's heart that finally worked.
Katsumata made certain that there was no bleeding, then meticulously closed the chest.
"Never been done before," he said, looking over at me. Soon afterwards Becky came down to the theatre in shock. After the encounter at the theatre door, she believed Kirsty had died. She put her hand on her baby's little foot and exclaimed, "It's warm. It's never been warm." When she started to cry I left. It had been a long day.
We followed Kirsty carefully over the following ten years, using echocardiography to watch her heart develop. She was a perfect little girl, happy, outgoing and energetic, the only clue to her extraordinary internal metamorphosis being the faint stripe up the middle of her chest.
When we felt she was mature enough to discuss it, we asked for her permission to carry out a magnetic resonance imaging scan to show us how the remodelled heart had developed. What we found was quite extraordinary. Apart from the double-orifice mitral valve her heart appeared normal, as did her new left coronary artery. Only the thin nest of scars showed the position of the line of stitches up the heart. Remarkably, all other scar tissue had disappeared. The whole inner lining of her left ventricle had been pure white scar tissue – now all gone.
This provided some of the first evidence that an infant's own cardiac stem cells can regenerate heart muscle and actually remove fibrous tissue. Adult hearts cannot recover in the same way. But what if we could identify and culture stem cells that could do just this for an adult heart? One day I'd find out.
Now aged eighteen, Kirsty is a vivacious and athletic teenager. Had she died we'd never have known about this exciting possibility for heart regeneration.
Westaby must have the last words:


No comments:
Post a Comment